What is Urinary tract infection or UTI?
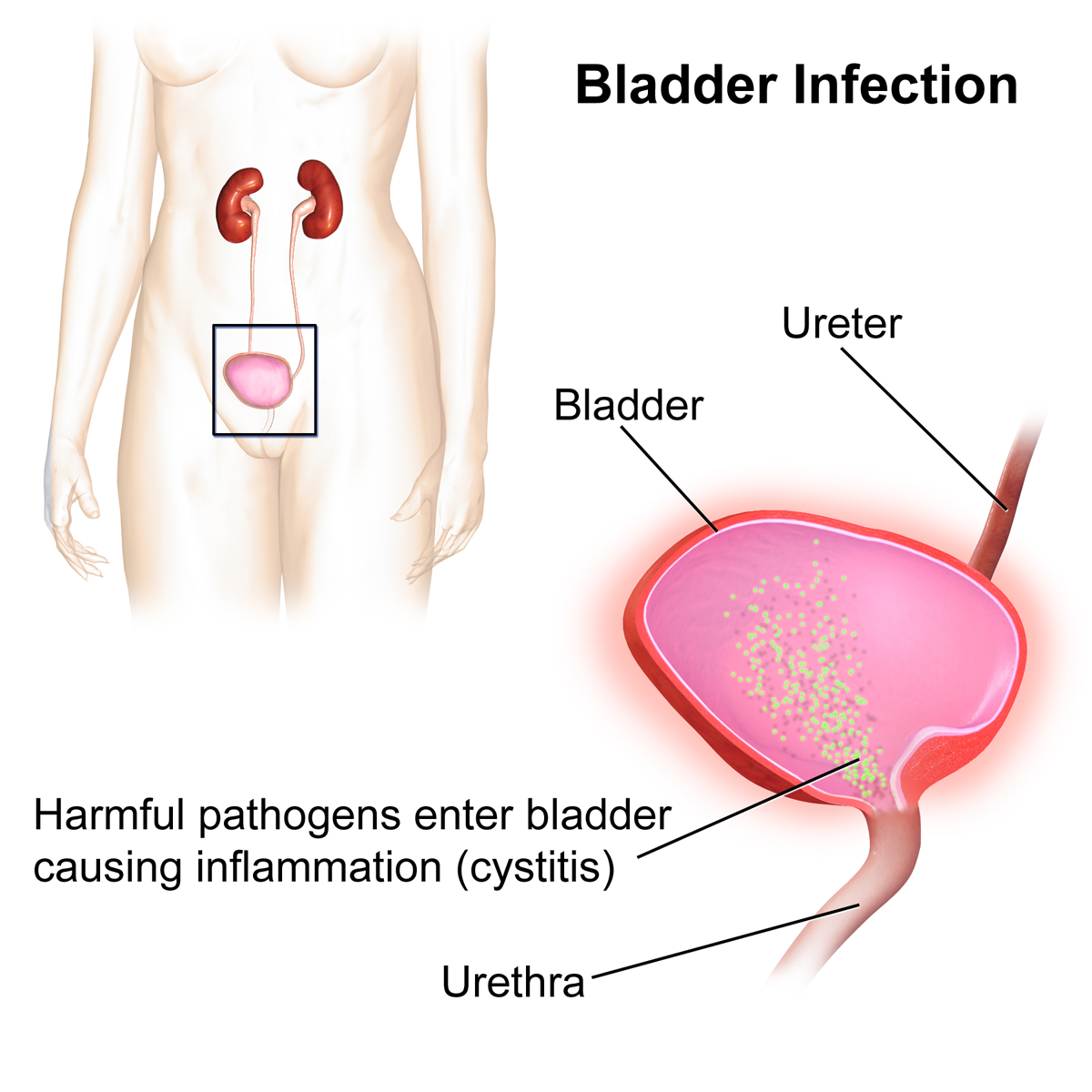
Urinary tract infections (UTIs) can affect different parts of the urinary tract, bladder (cystitis), urethra (urethritis) or kidneys (kidney infection).
What are the symptoms of Urinary tract infection?
Pee more than usual, or suddenly
Pain or discomfort while peeing
Smelly or cloudy urine
Blood in the urine
Discomfort in the abdomen (tummy), or sides of the abdomen (flanks)
Feeling tired, chills and fever
In older patients, they may be confused or agitated
What should I do if I have symptoms of Urinary tract infection?
Consult your healthcare provider.
How is Urinary tract infection diagnosed and treated?
Your healthcare provider will perform a physical exam, Lab tests, urine tests.
Men may have a swab taken from the tip of the penis.
How is urinary tract infection treated?
Urinary tract infection is treated with antibiotics.
How do I prevent urinary tract infection?
Finish antibiotics as prescribed completely, even when you feel better with a few pills.
Drink plenty of fluids.
Wipe from front to back when you go to the toilet.
Try to empty your bladder fully when you pee
Take showers instead of bath
Personal hygiene, Loose cotton underwear
Pee, wash with soap and water before and after sex
Change diapers regularly.
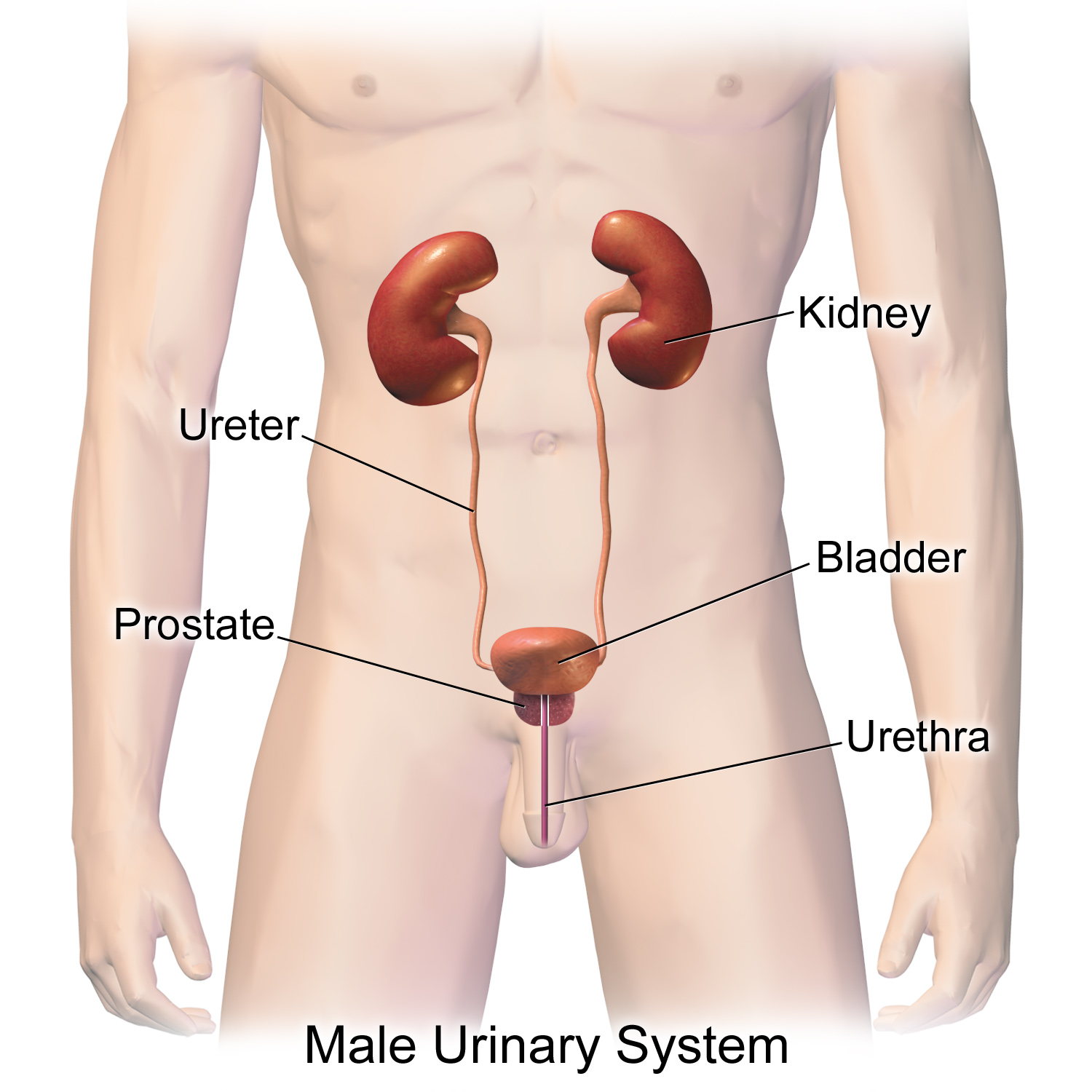
Location of Urinary tract